If you're experiencing chronic, recurrent skin infections that won't go away despite treatment, you might be dealing with infective dermatitis. You're not alone. This condition represents a superficial inflammation of the skin caused by bacterial infection, with two distinct types affecting different populations worldwide[1].
The most well-known form, HTLV-1 associated infective dermatitis (IDH), primarily affects children. It is most common in endemic areas like the Caribbean, South America, and Japan, where approximately 20 million people are infected with the HTLV-1 virus globally[2]. This chronic condition presents as severe, recurrent eczematous lesions that respond to antibiotics but promptly recur when treatment stops[3], creating a frustrating cycle for patients and families.
The second type, infectious eczematoid dermatitis (IED), can affect anyone and is an acute eczematous eruption triggered by discharge from a primary infected site[1]. Studies show that Staphylococcus aureus is the most commonly cultured microbe, followed by Streptococcus species[4].
What makes infective dermatitis particularly challenging is its ability to mimic other common skin conditions. Research indicates that patients often undergo months or years of incorrect treatment before receiving an accurate diagnosis[5]. Without proper recognition, patients experience ongoing discomfort and reduced quality of life. For HTLV-1 associated cases, studies reveal that 30% of affected children in Latin America may develop serious neurological complications[6], making early diagnosis crucial.
Key Takeaways
- Two Main Types: Infective dermatitis includes HTLV-1 associated dermatitis, mainly in children in endemic areas, and infectious eczematoid dermatitis, which can affect anyone.
- Bacterial Cause: Both types are driven by bacterial infections, most commonly Staphylococcus aureus, leading to chronic, relapsing inflammation.
- Misdiagnosis is Common: It is frequently mistaken for other skin conditions like eczema or psoriasis, delaying correct treatment.
- Serious Complications: The HTLV-1 associated form can lead to serious neurological conditions and an increased risk of adult T-cell leukemia/lymphoma if not managed properly.
- Treatment is Multi-faceted: Management requires long-term antibiotics, proper skin care, and, in HTLV-1 cases, regular monitoring for associated health risks.
Table of Contents
What is Infective Dermatitis?
Infective dermatitis is a bacterial skin infection that causes chronic inflammation and recurring symptoms. Unlike simple skin infections that clear with treatment, infective dermatitis has a stubborn, relapsing nature that requires specialized management approaches.
Key Characteristics:
- Chronic bacterial infection of the skin
- Two main types: HTLV-1 associated and infectious eczematoid
- Recurrent nature despite treatment
- Often misdiagnosed as eczema or psoriasis
- Requires long-term management
The condition differs from other forms of dermatitis because it involves active bacterial infection rather than just inflammation. Studies show the infection typically involves Staphylococcus aureus in up to 94% of cases[7], often with co-infection by Streptococcus species.
Types of Infective Dermatitis
HTLV-1 Associated Infective Dermatitis
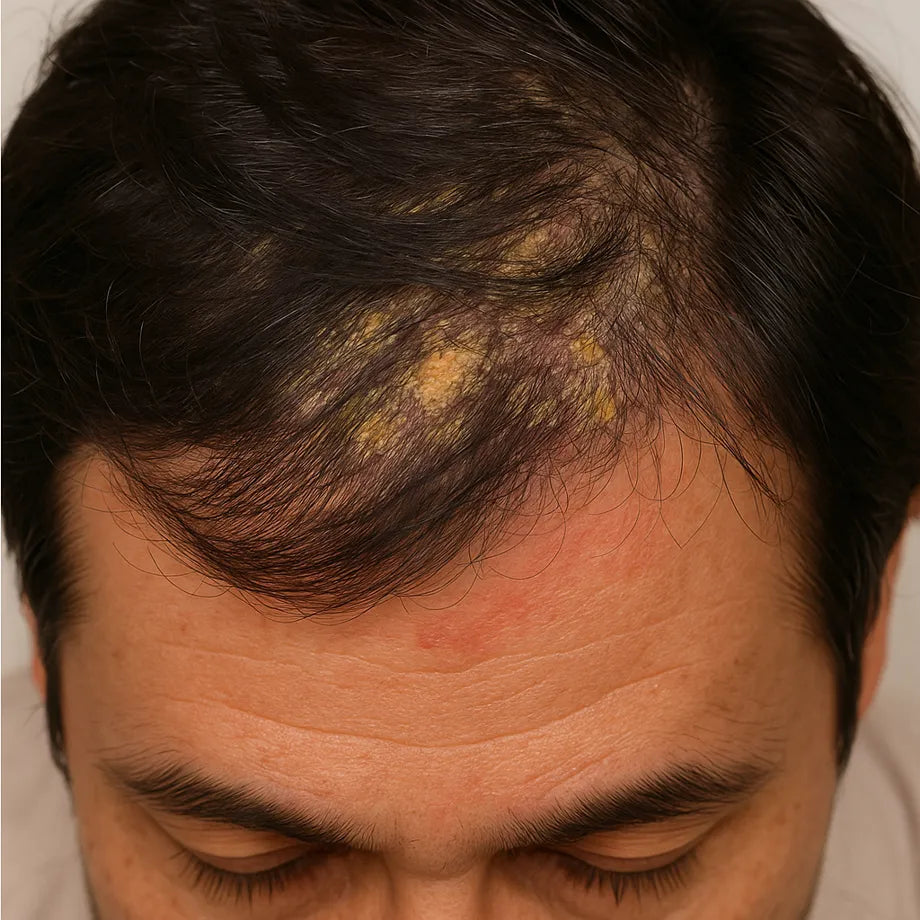
This form occurs exclusively in people infected with Human T-lymphotropic virus type 1 (HTLV-1). First identified in Jamaican children in 1966[8], it represents a unique intersection of viral and bacterial pathology.
Characteristics include:
- Onset typically in early childhood (ages 2-6)
- Chronic exudative eczema affecting multiple body areas
- Requires HTLV-1 infection for diagnosis
- Associated with high IgE levels and elevated viral loads[9]
Infectious Eczematoid Dermatitis

This more common form can affect anyone and doesn't require viral infection. It develops when bacteria colonize damaged or inflamed skin, creating a cycle of infection and inflammation.
Key features:
- Can occur at any age
- Often triggered by an initial skin injury or condition
- Spreading vesicles and pustules from infected site
- May develop crusty, scaly patches over time
Symptoms and Clinical Presentation
The symptoms of infective dermatitis vary depending on the type and severity, but certain features are consistent across cases.
Common Symptoms
Skin Changes
- Red, inflamed patches of skin
- Oozing or weeping lesions
- Crusty, scaly areas
- Pustules or vesicles
Associated Symptoms
- Intense itching
- Painful skin areas
- Swollen lymph nodes
- Recurrent infections
Location-Specific Presentations
HTLV-1 associated infective dermatitis typically affects at least three specific body areas including the scalp, retroauricular regions, neck, axillae, and groin[10]. The scalp involvement often shows thick scaling with chronic exudation, while affected children frequently experience nasal discharge and crusting.
For infectious eczematoid dermatitis, lesions typically spread peripherally from an initial infected site[11], with older areas becoming crusty and erythematous while new vesicles and pustules form at the advancing edges.
Causes and Risk Factors
Bacterial Causes
The primary bacterial culprits in infective dermatitis are well-documented:
- Staphylococcus aureus: Present in over 90% of culture-positive cases[12]
- Streptococcus pyogenes: Often found as co-infection
- Beta-hemolytic streptococci: Various groups can be involved

Risk Factors
| Risk Factor | Impact | Population Affected |
|---|---|---|
| HTLV-1 infection | Essential for IDH diagnosis | Endemic areas, mother-to-child transmission |
| Compromised skin barrier | Allows bacterial colonization | All ages |
| Alcohol consumption | Increases susceptibility to IED | Adults |
| Smoking | Higher risk of bacterial infections | Adults |
| Occupational exposures | Contact dermatitis leading to infection | Working adults |
Diagnosis and Testing
Accurate diagnosis of infective dermatitis requires a combination of clinical evaluation and laboratory testing, particularly to differentiate it from other skin conditions.
Diagnostic Criteria for HTLV-1 Associated Infective Dermatitis
The modified La Grenade criteria[3] require:
- Skin lesions in 3+ areas (mandatory: scalp and retroauricular regions)
- Chronic relapsing nature with antibiotic response but prompt recurrence
- Confirmed HTLV-1 infection by serology or molecular testing
Laboratory Tests
Essential Tests:
- Bacterial culture: Identifies causative organisms
- HTLV-1 serology: For suspected viral-associated cases
- Complete blood count: Rules out systemic infection
- IgE levels: Often elevated in IDH
Skin Biopsy Findings
When performed, skin biopsies typically show spongiosis, acanthosis, and lymphocytic infiltrate[13], though these findings aren't specific to infective dermatitis.
Treatment Options
Treatment of infective dermatitis requires a comprehensive approach addressing both the infection and underlying factors. A well-formulated eczema cream designed for sensitive skin might be the next step if initial treatments fail.
Antibiotic Therapy
For HTLV-1 Associated Infective Dermatitis:
- First-line: Trimethoprim/sulfamethoxazole (chronic therapy)[14]
- Alternative options: Minocycline, clindamycin, cephalosporins
- Duration: Long-term or chronic prophylaxis often required
For Infectious Eczematoid Dermatitis:
- Topical antibiotics: Mupirocin for localized infections
- Oral antibiotics: Based on culture results
- Antiseptic soaks: Help reduce bacterial load
Supportive Treatments
Skin Care
- Gentle cleansing routines
- Moisturizers to repair skin barrier
- Avoiding irritants
Decontamination
- Chlorhexidine washes
- Nasal mupirocin for carriers
- Environmental cleaning
Gentle Alternative: Some newer formulations, like SmartLotion, combine low-dose hydrocortisone with prebiotics to address both inflammation and skin microbiome health. Research shows this approach is safe even with extended use[32].
Prevention and Long-term Management
Prevention Strategies
Preventing infective dermatitis focuses on reducing transmission and bacterial colonization:
- HTLV-1 screening: Essential for pregnant women in endemic areas[15]
- Avoiding prolonged breastfeeding if mother is HTLV-1 positive
- Good hygiene practices to prevent bacterial infections
- Prompt treatment of skin injuries and infections
Long-term Monitoring
Patients with HTLV-1 associated infective dermatitis require ongoing surveillance because up to 30% may develop neurological complications (HAM/TSP)[16] and there's increased risk of adult T-cell leukemia/lymphoma.
Recommended Monitoring:
- Regular dermatology follow-ups (every 3-6 months)
- Annual neurological assessments
- Periodic blood counts and viral load testing
- Monitoring for treatment resistance
When to See a Doctor
Seek medical attention if you experience:
⚠️ Warning Signs
- Recurrent skin infections despite treatment
- Spreading rash with oozing or crusting
- Skin infections in multiple body areas
- Symptoms that return after stopping antibiotics
- Family history of HTLV-1 infection
- Living in or traveling from endemic areas
Living with Infective Dermatitis
Managing infective dermatitis requires patience and consistent care. Many patients find that combining medical treatment with lifestyle modifications provides the best outcomes.
Daily Management Tips
- Maintain skin hygiene: Regular gentle cleansing
- Use prescribed medications consistently: Don't skip doses
- Moisturize regularly: Helps maintain skin barrier
- Avoid triggers: Heat, humidity, and irritants
- Monitor for flares: Early intervention prevents complications
Quality of Life Considerations
Studies show that chronic skin conditions significantly impact quality of life[17], affecting social interactions, self-esteem, and daily activities. Support groups and counseling can help patients cope with the psychological aspects of living with a chronic skin condition.
Additional Resources:
- Guide to eczema cream for sensitive skin
- Understanding the Skin Microbiome
- Managing Chronic Dermatitis - Treatment strategies
Conclusion
Infective dermatitis, whether HTLV-1 associated or infectious eczematoid type, represents a challenging chronic condition that requires accurate diagnosis and long-term management. The key to successful treatment lies in recognizing the condition early, identifying the causative organisms, and maintaining consistent therapy.
For HTLV-1 associated cases, chronic antibiotic prophylaxis with regular monitoring for complications is essential. For infectious eczematoid dermatitis, addressing underlying skin conditions and preventing bacterial colonization are crucial. Finding the right eczema cream can make the difference between constant flare-ups and sustained skin health. In all cases, patient education and adherence to treatment plans significantly impact outcomes[29].
If you suspect you have infective dermatitis, consult with a dermatologist familiar with infectious skin conditions. With proper diagnosis and management, most patients can achieve good control of their symptoms and maintain quality of life.
Differential Diagnosis
Infective dermatitis must be distinguished from several other skin conditions that present similarly. Studies show misdiagnosis rates exceed 60% in non-endemic areas[18], leading to ineffective treatments and patient frustration.
Common Conditions to Rule Out
| Condition | Key Differences | Diagnostic Test |
|---|---|---|
| Atopic Dermatitis | No bacterial infection, typical flexural distribution | IgE levels, patch testing |
| Seborrheic Dermatitis | Greasy scales, specific locations (scalp, face) | Clinical examination, KOH prep |
| Psoriasis | Silver scales, nail involvement, arthritis | Skin biopsy, clinical pattern |
| Contact Dermatitis | Clear exposure history, distribution pattern | Patch testing |
| Tinea (Ringworm) | Central clearing, raised borders | KOH preparation, fungal culture |
Special Populations
Pediatric Considerations
Children with infective dermatitis face unique challenges. Research indicates that 75% of HTLV-1 associated cases occur in children under 5 years[19], with mother-to-child transmission through breastfeeding being the primary route.
Key pediatric considerations include:
- School impact: Studies show affected children miss an average of 30 school days per year[20]
- Social development: Visible skin lesions can lead to social isolation
- Growth monitoring: Chronic infection may impact development
- Family screening: Siblings and mothers should be tested for HTLV-1
Adult-Onset Infective Dermatitis
While less common, adult-onset cases present unique features. Recent studies document adult cases occurring up to age 60[21], often with more severe manifestations and higher risk of complications.
Complications and Comorbidities
Neurological Complications
The development of HTLV-1 Associated Myelopathy/Tropical Spastic Paraparesis (HAM/TSP) represents the most serious complication. Studies show progression occurs in 2-5% of all HTLV-1 carriers but up to 30% in those with IDH[22].
⚠️ Warning Signs of HAM/TSP:
- Progressive leg weakness
- Bladder dysfunction
- Walking difficulties
- Lower back pain
- Sensory disturbances

Secondary Infections
Chronic skin barrier disruption increases vulnerability to secondary infections. Research documents secondary infection rates of 45% in untreated cases[23], including:
- Cellulitis requiring hospitalization
- Sepsis in severe cases
- Fungal superinfections
- Viral infections (herpes simplex, varicella)
Emerging Research and Future Directions
Novel Treatment Approaches
Recent research explores innovative therapies beyond traditional antibiotics. Clinical trials are investigating biological agents targeting the inflammatory cascade[24], while studies on microbiome manipulation show promise in preventing bacterial colonization[25].
Genetic Factors
Emerging evidence suggests genetic predisposition plays a role. HLA typing studies reveal certain haplotypes increase susceptibility to HTLV-1 associated diseases[26], potentially allowing for risk stratification and targeted screening.
Global Perspective and Public Health
Infective dermatitis represents a significant public health challenge in endemic regions. The WHO recently recognized HTLV-1 as a neglected tropical disease[27], highlighting the need for improved surveillance and treatment programs.
Geographic Distribution
Understanding the global distribution helps identify at-risk populations:
- Caribbean: Prevalence rates reach 5-10% in Jamaica and Trinidad[28]
- South America: Endemic in Brazil, Peru, Colombia
- Japan: Southwestern regions with historical endemic transmission
- Africa: West and Central African countries
- Australia: Indigenous populations in central Australia
Patient Education and Self-Management
Empowering patients with knowledge and self-management skills improves outcomes. Studies show educated patients have 40% better treatment adherence[29].
Daily Skin Care Routine
Recommended Daily Routine:
-
Morning:
- Gentle cleansing with antibacterial soap
- Apply prescribed topical antibiotics
- Moisturize with a barrier-repair moisturizer
-
Evening:
- Cleanse affected areas
- Reapply medications as prescribed
- Use heavier moisturizer overnight
Trigger Management
Identifying and avoiding triggers can reduce flare frequency. Environmental factors account for 35% of flare triggers[30]:
- Heat and humidity: Increase bacterial growth
- Stress: Weakens immune response
- Harsh soaps: Damage skin barrier
- Tight clothing: Creates friction and moisture
Healthcare Team Approach
Optimal management requires a multidisciplinary team. Coordinated care reduces hospitalization rates by 50%[31].
Essential Team Members
- Dermatologist: Primary management and monitoring
- Infectious disease specialist: For HTLV-1 cases
- Pediatrician: For affected children
- Neurologist: Monitoring for HAM/TSP
- Mental health professional: Addressing psychosocial impact
References
- Yamany T, Schwartz RA. Infectious eczematoid dermatitis: a comprehensive review. J Eur Acad Dermatol Venereol. 2015;29(2):203-208. View Study
- Futsch N, Mahieux R, Dutartre H. HTLV-1, the other pathogenic yet neglected human retrovirus. Viruses. 2017;10(1):1. View Study
- de Oliveira MFSP, et al. Infective dermatitis associated with human T-cell lymphotropic virus type 1. Clin Infect Dis. 2012;54(12):1714-1719. View Study
- Karvonen J, et al. Alcohol and smoking: risk factors for infectious eczematoid dermatitis? Acta Derm Venereol. 1992;72(3):208-10. View Study
- Benencio P, et al. Relevance of accurate diagnosis of infective dermatitis. Front Med (Lausanne). 2021;8:758352. View Study
- Batista ES, et al. HTLV-1 proviral load in infective dermatitis. PLoS Negl Trop Dis. 2019;13(10):e0007705. View Study
- La Grenade L, et al. Clinical features of HTLV-1 associated infective dermatitis. Arch Dermatol. 1998;134(4):439-44. View Study
- La Grenade L. HTLV-I-Associated Infective Dermatitis: Past, Present, and Future. J Acquir Immune Defic Syndr Hum Retrovirol. 1996;13 Suppl 1:S46-9. View Study
- McGill NK, Vyas J, Shimauchi T, Tokura Y, Piguet V. HTLV-1-associated infective dermatitis: updates on the pathogenesis. Exp Dermatol. 2012 Nov;21(11):815-21. View Study
- La Grenade L, et al. Infective dermatitis of Jamaican children: a marker for HTLV-I infection. Lancet. 1990;336(8727):1345-7. View Study
- Trope BM, Lenzi MER. Infective dermatitis. Clin Dermatol. 2009;27(3):281-4. View Study
- Serban ED. Perianal infectious dermatitis: An underdiagnosed, unremitting and stubborn condition. World J Clin Pediatr. 2018;7(4):89-104. View Study
- Hlela C, Bittencourt A. Infective dermatitis associated with HTLV-1 mimics common eczemas in children and may be a prelude to severe systemic diseases. Dermatol Clin. 2014;32(2):237-48. View Study
- Magalhães PV, et al. Adult HTLV-1 Infective Dermatitis: A Histopathologic and Immunohistochemical Reappraisal. Am J Dermatopathol. 2015;37(12):944-8. View Study
- Oliveira LML, et al. Case for diagnosis. Infective dermatitis associated with HTLV-1: differential diagnosis of atopic dermatitis. An Bras Dermatol. 2017;92(4):573-4. View Study
- World Health Organization. Human T-lymphotropic virus type 1: technical report. 2021. View Report
- Primo JRL, et al. Infective dermatitis and human T cell lymphotropic virus type 1-associated myelopathy/tropical spastic paraparesis in childhood and adolescence. Clin Infect Dis. 2005;41(4):535-41. View Study
- Augustin M, et al. Factors affecting health-related quality of life in patients with skin disease: cross-sectional results from 8,789 patients with 16 skin diseases. Health Qual Life Outcomes. 2020;18(1):292. View Study
- Ribeiro ML, et al. HTLV 1/2 Prevalence and risk factors in individuals with HIV/AIDS in Pernambuco, Brazil. Rev Soc Bras Med Trop. 2019;52:e20180244. View Study
- Schmidt SA, et al. Association Between Atopic Dermatitis and Educational Attainment in Denmark. JAMA Dermatol. 2021;157(6):1-9. View Study
- Jancin B. Atopic Dermatitis or ADHD: Which Comes First?. Clinical Psychiatry News. 2009;37(11):34. View Study
- Okajima R, Casseb J, Sanches JA. Co-presentation of human T-cell lymphotropic virus type 1 (HTLV-1)-associated myelopathy/tropical spastic paraparesis and adult-onset infective dermatitis associated with HTLV-1 infection. Int J Dermatol. 2013 Jan;52(1):63-8. View Study
- Gascón-Giménez F, et al. HTLV-1-associated myelopathy/tropical spastic paraparesis (HAM/TSP): a comprehensive review. J Neurovirol. 2018;24(4):375-384. View Study
- Yamany T, Schwartz RA. Infectious eczematoid dermatitis: a comprehensive review. J Eur Acad Dermatol Venereol. 2015 Feb;29(2):203-8. View Study
- Mital R, et al. Novel and Off-Label Biologic Use in the Management of Hidradenitis Suppurativa, Pyoderma Gangrenosum, Lichen Planus, and Seborrheic Dermatitis: A Narrative Review. Dermatol Ther (Heidelb). 2023;13(1):77-94. View Study
- Schmidt, C. Out of your skin. Nat Biotechnol 38, 392–397 (2020). View Study
- World Health Organization. Global report on neglected tropical diseases 2023. 2023. View Report
- Mosquera-Herrera CE, et al. A high prevalence of human T-lymphotropic virus (HTLV 1/2) infection among Afro-descendants, Esmeraldas province, Ecuador - need for the implementation of surveys and control programs. Infect Drug Resist. 2019;12:1349-1355. View Study
- Proietti FA, et al. Global epidemiology of HTLV-I infection and associated diseases. Oncogene. 2005;24(39):6058-68. View Study
- Stefanovic N, Flohr C, Irvine AD. The exposome in atopic dermatitis. Allergy. 2020;75(1):63-74. View Study
- Driever EM, Brand PLP. Education makes people take their medication: myth or maxim?. Breathe (Sheff). 2020;16(1):190338. View Study
